| visit: www.infertilitytutorials.com |
|
Immunologic Cells and Antibodies
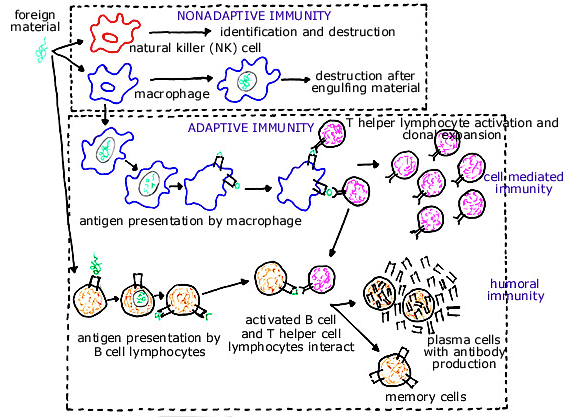
The primary function of the immune system is to protect oneself (self) from outside (foreign or infectious) organisms or ones own toxic products (collectively nonself). Nonadaptive immunity utilizes cells that identify nonself structures and destroy (or remove) them directly without developing an enhanced future sensitivity to these structures. The cells that are employed within the nonadaptive (innate) immune system are natural killer cells (NK cells) and macrophages. It appears that the activation of NK cells is (at least partially) suppressed by T suppressor cells (a type of lymphocyte) such that a reduced number of T suppressor cells within a tissue are associated with greater local activity of NK cells. Adaptive immunity identifies foreign (nonself) material, mediates its attack against these structures using a type of cell (lymphocyte) that is able to produce very specific proteins (antibodies) designed to recognize a particular foreign stimulus (antigen), and these antibodies recognize and bind to the foreign material (stimulus) to initiate a cascade of events that eventually destroys the foreign substance. The initial response to a particular foreign material is slow, but the immune system remembers its prior attacks so that subsequent immune response(s) to the same foreign material is much more rapid. The substances that can illicit an immune reaction (antigens) are initially identified as nonself and are (usually) engulfed by macrophages, the antigen is then processed within these cells, and finally the processed fragments of the original antigen are presented by these cells on their cell surface. These cells are collectively called antigen presenting cells (APCs). APCs then trigger the cell mediated and/or antibody mediated (humoral) immune systems. In cell mediated immunity, APCs bind to helper T lymphocytes (which learn to specifically recognize the particular antigen fragment that is presented). Binding the helper T cell to the APC results in clonal expansion (an exponential increase in number) of the specific helper T cells. The bound helper T cell - APC complex then is able to eradicate the foreign material that initiated this cascade of events. In humoral (antibody mediated) immunity, antigens are processed within B lymphocytes and fragments of these antibodies are presented on their surface (much like the events occurring within APCs). Helper T lymphocytes then bind to the B lymphocytes (presenting the antibody fragments) and this interaction allows the B lymphocytes to undergo clonal expansion (an exponential increase in number). These expanding B lymphocytes can then differentiate (mature) into either plasma cells (cells that last for only a few days and are highly specialized to produce large amounts of antibodies) or memory cells (long lasting cells that do not produce antibodies but rather remain within the circulation and are primed to rapidly respond to repeat exposure to the same antigen). Antibodies elaborated by the plasma cells bind the antigen and this initiates events that eradicate it. IMMUNE TOLERANCE The DNA within a fertilized egg normally has 23 pairs of chromosomes, one of each pair from the father and one of each pair from the mother. The DNA within a cell regulates the expression of cell surface antigens on the outside of the cell. Since some of the DNA within a fertilized egg is paternal (from the father) the antigens that are formed on the surface of the growing placental cells are not entirely maternal. In theory, the paternal antigens that are expressed on the surface of the implanting placental cells should routinely be identified by the maternal immune system as nonself and this should stimulate immunologic rejection of the pregnancy. The way in which the fetal-placental unit escapes immunologic attack and destruction by the maternal immune system is not clearly understood. The failure of the maternal immune system to become activated against a pregnancy within the uterus is called tolerance and the placental implantation site within the uterus is referred to as an immunologically privileged site. A lack of immune tolerance may be the cause of some recurrent pregnancy losses. A variety of theories regarding an immune mechanism (eg., involving sharing of HLA types, decreased numbers of blocking antibodies, enhanced natural killer cell activation) have been proposed and yet none of these has been generally accepted. At the present time, the diagnosis of this cause for recurrent pregnancy losses remains one of exclusion (all other causes have been ruled out, leaving this as one of the possibilities). | |||||||||||